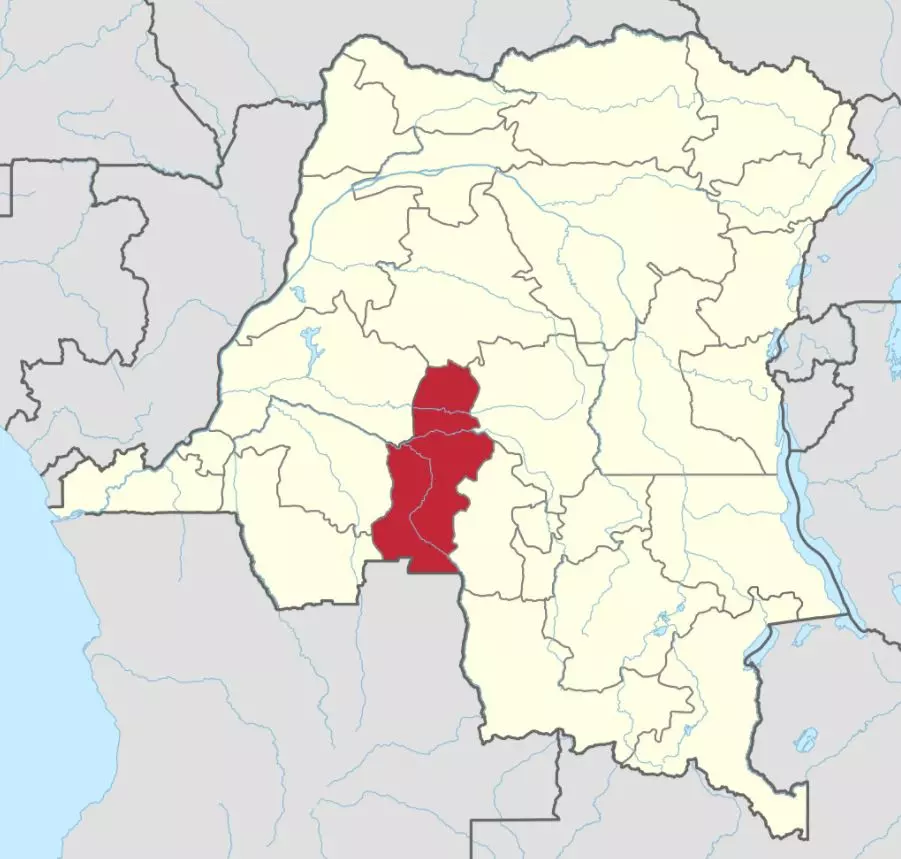
Original work:NordNordWest - CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=47013327
Although the current epidemic peaked in late September 2017 and national case numbers have gradually decreased, certain provinces such as South Kivu, Kasaï, Kongo Central, Lualaba and Kinshasa still struggled to control cholera outbreaks as of mid-December.
The cholera outbreaks in the western provinces, such as Kasaï, are especially worrying as these zones are non-endemic for cholera and have thus relatively limited experience and capacity to control and prevent outbreaks. Ever since the onset of the outbreak in Kasaï in early October 2017, the situation has been critical in certain health zones. In the Kasaï health zone of Dekese, which has been heavily affected by cholera, the CFR was 41.2% in early December and 22.2% in late December 2017. Factors behind the significantly elevated number of cholera-related deaths in the Dekese included a lack of standard support structures, poorly experienced staff, and unsanitary burial practices. The situation in Kasaï Province has also been compounded by the displacement of more than 1.4 million civilians due to escalating violence.
Following a statement from the Minister of Health, Dr. Oly Ilunga Kalenga, on December 27, 2017, the government reacted quickly and immediately initiated community support measures and bolstered epidemiological surveillance in the affected areas.
To quickly avert further preventable deaths, a PNECHOL-MD rapid response team was dispatched to Dekese. To reach the difficult to access area, the team crossed the Sankuru River by boat and then walked 10 km on foot in the forest and the hills of Mvusengando. Once reaching Dekese, the team conducted initial investigations and raised community awareness. The World Health Organization has already sent the first shipment of medication and additional shipments are planned.
